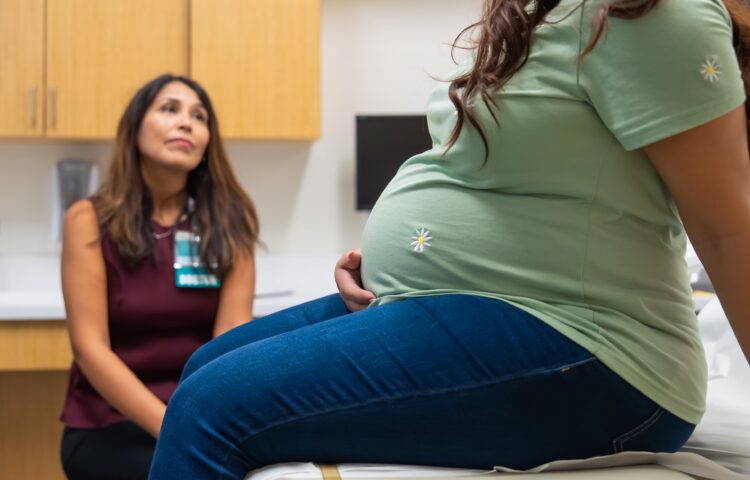
Discovering you’ve been referred to a maternal-fetal medicine (MFM) specialist can feel overwhelming at first, but understanding this pivotal step in your prenatal care journey can transform uncertainty into empowerment. Whether you’re facing a high-risk pregnancy, managing a chronic condition, or simply need specialized monitoring, an MFM specialist brings advanced expertise to support both you and your growing baby.
Here’s what that referral means and what you can expect next.
What is Maternal-Fetal Medicine (MFM)?
Maternal-fetal medicine specialists are dual-board-certified obstetricians with advanced training in high-risk pregnancy, and many people also use the term high-risk obstetrician for MFM specialists. There’s an additional layer to the MFM meaning beyond just the acronym. The hyphen in maternal-fetal medicine represents medicine that treats maternal and fetal health as fundamentally linked. It’s an approach to care that recognizes you can’t truly focus on outcomes for the baby without also caring for the mother, and vice versa.
Is an MFM specialist the same as a perinatologist?
If you’re asking yourself, “What is a perinatologist versus an MFM specialist?,” they’re actually the same thing. You’ll hear both terms used interchangeably throughout your care. Whatever the terminology, you’ll be referred to an MFM if there’s an increased risk in your pregnancy — whether that’s due to a maternal health condition, a concern with your baby, or both.

Why would my obstetrician refer me to an MFM specialist?
If your obstetrician (OB) mentions referring you to an MFM specialist, you might naturally wonder, “Why me?” The truth is, MFM referrals are more common than you think, and they happen for many reasons — some before you even conceive, others during your first trimester, and still others later in pregnancy as your baby grows. Whether it’s due to a preexisting health condition, something that developed during pregnancy, or findings from routine testing, an MFM referral simply means your care team wants to bring in extra expertise to support you and your baby.
Here are some of the most common reasons your OB might bring an MFM specialist onto your care team.
Early in pregnancy if you have any of these conditions:
- High blood pressure, you had hypertension before getting pregnant
- IVF pregnancy, you conceived through in vitro fertilization
- Diabetes or prediabetes, you have Type 1, Type 2 diabetes, or higher-than-normal blood sugar levels
- Heart condition, a cardiac problem that needs monitoring during pregnancy
- Kidney disease, ongoing kidney problems
- Thyroid disorder, your thyroid is overactive (hyperthyroidism) or underactive (hypothyroidism)
- Autoimmune condition, such as lupus (SLE) or antiphospholipid syndrome (APLS)
- Higher BMI, body mass index is in a range that may require extra monitoring
- Severe asthma, asthma needs careful management during pregnancy
- History of stroke, you’ve had a stroke in the past
- Gastric bypass surgery, you’ve had weight loss surgery with significant weight loss
- Infection or exposure concerns, such as HIV, CMV (cytomegalovirus), or parvovirus
- Maternal age 35 or older, 35 years of age or older at your due date
- Seizure disorder, you have epilepsy or another condition that causes seizures
- Family or personal history of abnormal pregnancies or genetic conditions
Complications, symptoms, or test results during pregnancy:
- Cholestasis of pregnancy, a liver condition that causes intense itching, usually in late pregnancy
- Preeclampsia, high blood pressure that develops during pregnancy
- Gestational diabetes, diabetes that develops during pregnancy
- Preterm labor, signs that you might deliver before 37 weeks
- Severe morning sickness, hyperemesis gravidarum, where you can’t keep food or fluids down
- Bleeding during pregnancy, vaginal bleeding at any point in your pregnancy
- Amniotic fluid concerns, either too little (oligohydramnios) or too much (polyhydramnios) fluid around your baby
- Short cervix, your cervix is shorter than expected, which could increase preterm birth risk
- Water breaking early, membranes rupture before labor begins
- Twin pregnancy, you’re expecting twins, triplets or higher-order multiples
- Twin-to-twin transfusion syndrome (TTTS), twins sharing a placenta with unequal blood flow between them
- Poor fetal growth, baby isn’t growing at the expected rate (fetal growth restriction)
- Abnormal genetic screening results, tests like NIPT or a serum screening show potential concerns
- Structural abnormalities, ultrasound shows a possible birth defect or physical difference with your baby
If you’ve experienced any of these in a previous pregnancy:
- Premature birth, a baby delivered before 37 weeks
- Preeclampsia, dangerously high blood pressure during pregnancy
- Multiple miscarriages, loss of two or more pregnancies
- Cervical insufficiency, cervix opened too early (sometimes called cervical incompetence)
- Genetic condition or birth defect, a prior pregnancy had a chromosomal abnormality or structural issue

What happens at your first MFM appointment?
Upon arrival, the MFM team may begin by asking how much information you already have regarding the reason for the referral. Most primary obstetricians do a wonderful job explaining that the MFM doctor will now collaborate with them as part of a unified team. Moving forward, the MFM specialist will help guide your pregnancy care. They will recommend ultrasounds and suggest specific tests. If needed, they will also connect you with other specialists (like pediatric cardiologists or genetic counselors), advise on the best timing for your delivery, and discuss whether a vaginal birth or C-section would be safest for you and your baby.
Questions You May Want to Ask at Your First MFM Visit
It’s normal to have questions when meeting with an MFM specialist. Consider asking:
- Why was I referred, and what specific concerns are we monitoring?
- How often will I need ultrasounds or additional visits?
- Will I continue to see my regular OB, and how will you coordinate care?
- Are there lifestyle changes or precautions I should take?
- What symptoms should prompt me to call my care team right away?
What tests or monitoring might be recommended?
MFM specialists offer specialized testing to help you get information about your baby’s health. This includes chorionic villus sampling (CVS), which involves taking a small sample of placental tissue, and amniocentesis, where a small sample of amniotic fluid is obtained. Testing is then performed on the placental tissue or amniotic fluid to help determine the diagnosis in the fetus. Detailed ultrasounds are also performed and provide in-depth imaging to examine your baby’s development.
MFMs may suggest these diagnostic tests if screening tests like NIPT (non-invasive prenatal testing) show potential concerns, if ultrasound findings need clarification, or if there’s a family history of genetic conditions like cystic fibrosis (CF) or spinal muscular atrophy (SMA). Testing might also be recommended if you’ve had a previous child with a chromosomal or genetic condition, if you’re 35 or older at your due date, if you or your partner carry a chromosomal rearrangement, if it’s possible your baby may have been exposed to an infection, or if there are concerns about blood type incompatibility such as Rh factor or other antibody issues. These tests help guide your care and decision making.
When patients are referred to MFMs for any of the above, they typically first meet with a genetic counselor. In addition to meeting with a genetic counselor, an ultrasound and a consult with an MFM physician help to provide a comprehensive assessment of the pregnancy. After meeting with the MFM doctor, you can decide to move forward with diagnostic testing. CVS is completed between 11–13 weeks and an amniocentesis is offered after 16 weeks.
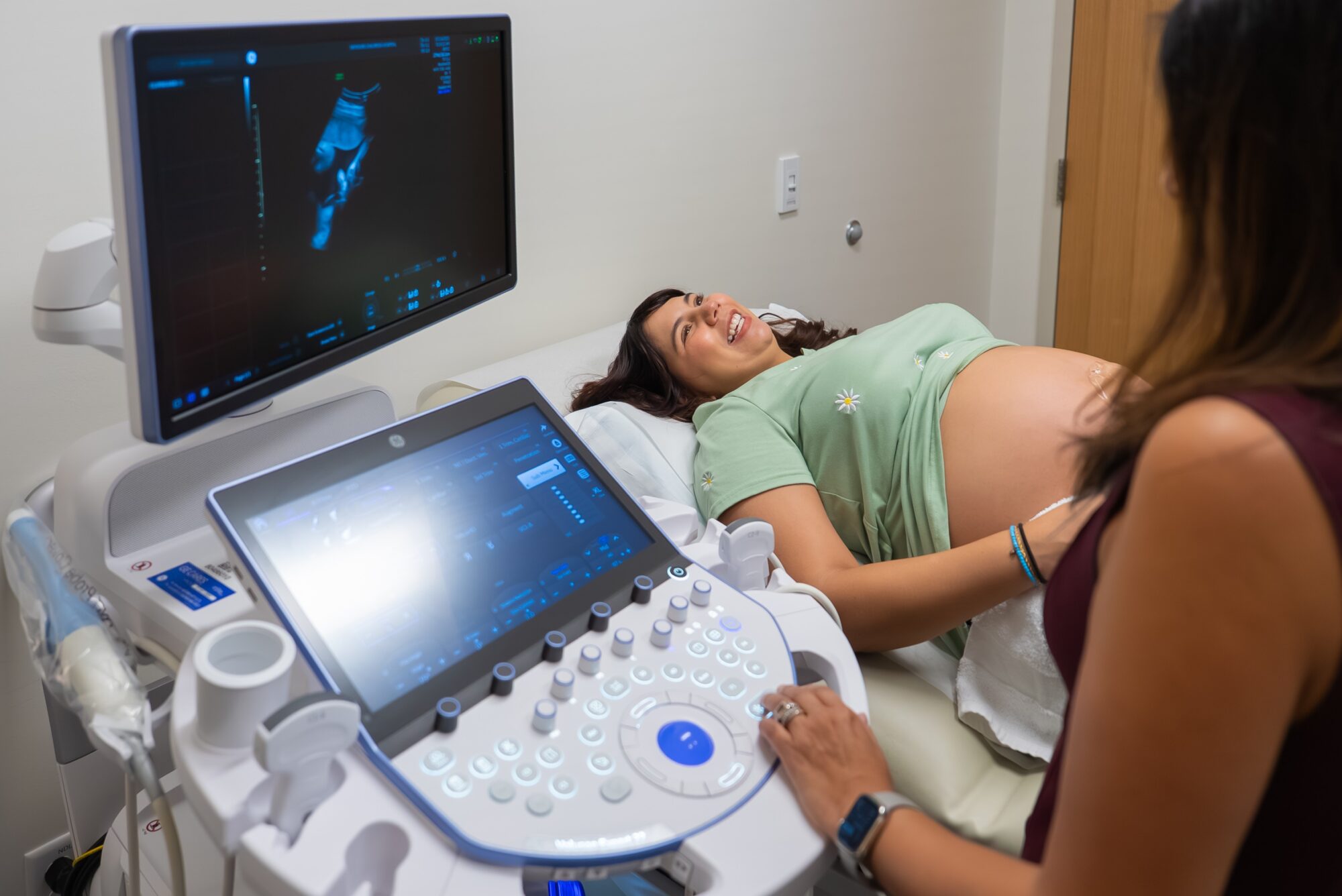
How your OB and MFM Work Together
MFM specialists are consultants who work closely with your obstetrician. Your obstetrician will coordinate your delivery and be there for the birth of your baby.
In most cases, your OB remains your primary pregnancy provider. Your MFM specialist offers additional expertise, monitoring, and recommendations. Together, they coordinate your care to support the healthiest possible outcome for you and your baby. They stay in communication about your test results and care plan so everyone is aligned on next steps and delivery planning.
In other words, your original OB/GYN usually delivers your baby, not your MFM specialist. Your MFM doctor is there throughout your pregnancy to do specialized monitoring and testing, so it creates an extended care team with your MFM advising and your OB implementing the care plan. Your OB continues as your primary pregnancy provider who performs the actual delivery.
What support is available to you and your baby?
Our Nemours Children’s MFM practice in Florida offers consultations with a diabetic educator, a nutritionist, a social worker, and multiple subspecialists at our fingertips as needed in your pregnancy. We also have dedicated perinatal coordinators who will follow you throughout the pregnancy for that one-on-one support if your baby is diagnosed with a congenital defect. The perinatal coordinators will be present at your subspecialty consultations (cardiology, urology, neurology, etc.) and available to you 24/7 should you have any questions or concerns.