When you’re told that you or your baby needs extended monitoring during a pregnancy complicated by a congenital anomaly or fetal diagnosis, it can feel overwhelming. This is especially true when you are cared for within a fetal center.
Perhaps you came in for a routine appointment, or maybe something unexpected happened that brought you to the hospital. Either way, the news that you’ll need to stay longer can stir up a whirlwind of emotions — worry, frustration, loneliness, and uncertainty about what lies ahead.
If you’re reading this, you may be facing this reality as an expectant parent within a fetal center right now, or perhaps you want to be prepared just in case. In a fetal center, the need for extended monitoring varies greatly, but it’s a precaution that helps ensure both you and your baby receive the specialized care you need, and there are ways to make this experience more manageable, both emotionally and logistically.
Let’s walk through what extended monitoring means, what you can expect, practical tips to prepare, and most importantly, how you can take care of yourself and your family during this challenging time.
What is extended fetal monitoring?
First, it’s important to understand that every pregnancy is unique. Within a fetal center, your care is truly individualized — no two moms or babies are exactly alike. What “monitoring” means for you will be tailored specifically to your pregnancy needs.
Extended monitoring can range from an additional 30 minutes of observation to several hours, or sometimes days, with a combination of ultrasounds and continuous or intermittent external fetal heart rate monitoring. Sometimes this monitoring can happen in an outpatient setting. Other times, staying in the hospital to gather more information —rather than just a snapshot in time — as an inpatient is the safest option. Plus, maternal monitoring or labs may also be a necessary part of the plan. In certain cases, increased outpatient monitoring or inpatient monitoring can be necessary until birth.

What is the purpose of inpatient extended fetal monitoring?
Your medical team may recommend an extended hospital stay with maternal and/or fetal monitoring for various reasons – all centered on keeping you and your baby (or babies) safe and close to the delivery team if a change in plan is warranted.
Maternal safety is paramount in these decisions, and extended monitoring ensures that both you and your baby are being watched closely.
What are some common reasons for additional monitoring?
Here’s a short list of reasons your fetal care team may recommend extended monitoring:
For the Baby (or Babies):
- Your care team needs a bit of extra reassurance to confirm that your baby’s status has not changed from baseline.
- Baby was napping or less active during a monitoring session (which is actually quite common!).
- An ultrasound showed a change from your baby’s typical routine that requires more information.
- You, the parent, reported a change in fetal movement that you discussed with your team.
- After a procedure, additional monitoring ensures the baby tolerated the procedure well and that the uterus isn’t contracting due to irritation from the procedure.
For the Pregnant Patient:
- An assessment for preterm labor.
- Preterm premature rupture of membranes (when your water breaks before 37 weeks without contractions).
- Monitoring for elevated blood pressure or other maternal concern based on clinical findings.
- You, the parent, have a new concern or symptom that warranted additional attention after discussion with your fetal center team.
Remember, these recommendations come from a place of caution and care. Your baby is, in many ways, “the boss,” and these precautions help ensure the best possible outcome for both of you.
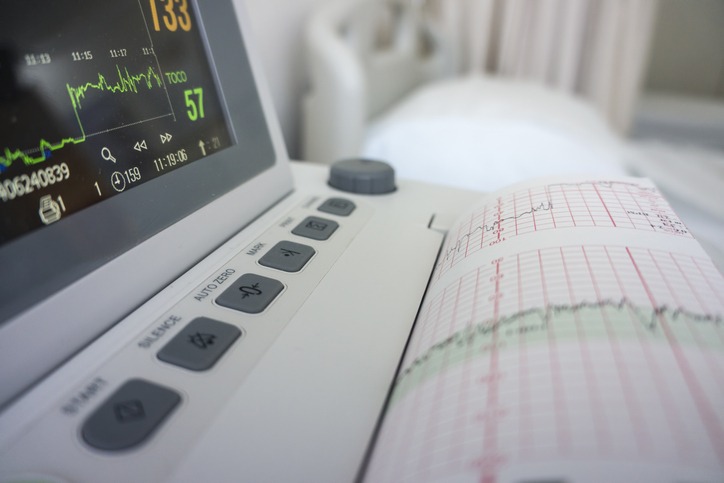
What can I expect during an extended hospital stay in a fetal care center?
Knowing what to expect can help ease some of the uncertainty. Here are the types of monitoring that may be part of your extended stay:
Monitoring
External Fetal Heart Rate Monitoring
During external fetal heart rate monitoring sessions, you’ll have two palm-sized circular monitors placed on your belly. One monitors changes in uterine tone (contractions), and the other tracks your baby’s heart rate. The heart rate tracing over time is actually a way that your baby can “talk” to the medical team and provide additional information.
- Continuous monitoring means the monitors are constantly transmitting information.
- Intermittent monitoring, which occurs for anywhere from 20 minutes to 1–4 hours (more common for longer stays), typically happens one to three times during waking hours.
Additional Monitoring
Your care team may perform these to help refine timing and frequency of various fetal assessments.
- Additional ultrasounds with “Doppler” waveforms to assess any changes. Dopplers are an assessment of blood flow within the baby and the umbilical cord. These waveforms can also be an added part of the story that help guide monitoring.
- Antenatal “Surveillance” is a type of monitoring that may be recommended in the outpatient or inpatient setting to provide more information about the baby’s status in utero. There are different types of antenatal fetal surveillance that you may hear about:
- NST: A nonstress test, generally performed after 28 weeks, is a 20–30-minute period of monitoring usually performed in the office.
- Biophysical profile (BPP), generally performed after 28 weeks, is an ultrasound performed to assess fetal status by way of 4 criteria (movement, tone, practice breathing and amniotic fluid level).
Results also help guide additional monitoring or detect changes in fetal status.
Your Care During the Stay
Hydration and Nutrition
Your medical team will advise if it’s OK to eat or drink. They may recommend that you do not have any fluid or food by mouth until further monitoring is performed. The medical team may also recommend IV fluids for hydration during the assessment. We know you’re hungry — it’s OK to ask frequently when you’re all clear to eat or drink.
Medications
If you’re admitted before 37 weeks, your team may recommend a course of antenatal steroids given by injection. The course includes two doses, usually 24 hours apart (helps with promoting lung maturity). In a fetal center, a steroid course can also be given to help treat a fetal diagnosis.

Your Care Team in a High-Risk Maternity Center
During your inpatient stay, you’ll meet these members of your care team:
- An experienced labor and delivery nurse
- An obstetrician (OB/GYN doctor) overseeing your care
- An anesthesiologist (if needed)
- A neonatologist (baby doctor) who cares for babies right at birth and in the Neonatal Intensive Care Unit (NICU) at your specialized center
- Psychosocial team professionals who will check in to provide information, resources, and support services tailored to your family’s specific needs
Ask Questions and Understand the Plan
If there is something going on around you that seems confusing or your care plan changes, don’t hesitate to ask why. Understanding the reasoning behind decisions can help reduce anxiety and frustration. Your care team wants you to feel informed and empowered.
Questions you might ask your care team or high-risk OB include:
- Why are we extending the monitoring period?
- What specific signs or changes are you watching for?
- What does this mean for my delivery timeline?
- What are the next steps in my care?
- How can I best support my baby during this time?
- Does anything change about the plan for the baby after birth if he/she comes earlier?
Remember, you are the center of your care team. If something feels different, you know yourself best — let your team know. They can often make adjustments to improve your experience.
“Pack and Plan” Pearls
You can’t always predict when or how long you’ll need to stay in the hospital, but there are steps you can take to make the experience smoother. There’s nothing wrong with being practical, and since the “baby is the boss,” try to stay one step ahead.
Keep a small bag of these essentials packed and ready:
- Change of clothes and underwear
- Comfortable socks (hospitals can be cold!)
- Glasses and contact lens case and solution
- Phone charger, watch charger, and any other essential electronics
- Toothbrush and basic toiletries
- Any compact comfort items that will help you feel more at home
If you have other children or dependents, having a “Just in Case” plan for your family can provide additional peace of mind:
- Identify who can care for siblings on short notice
- Share your plan with family and friends who can step in
- Keep important contact information and schedules easily accessible
- Prepare a list of your children’s routines, preferences, and important information for caregivers

Pearls for Extended Care
Patients who handle extended hospital stays most successfully share a few common characteristics that make all the difference in their experience.
Exercise Control Where You Can
No one can expect the unexpected, but having the ability to exercise a bit of control when something different is happening can be grounding. Whether it’s choosing your daily schedule, decorating your space, or deciding what you eat (when allowed), these small choices matter.
Utilize Available Support
Take advantage of psychosocial spaces and resources. These services exist specifically to help families through challenging times like this.
Stay Connected
Patients who maintain connections to their favorite things (support persons, children, family, friends, even pets) whether in person or virtually, tend to have better emotional outcomes.
Allow Yourself Grace
This is hard. Really hard. Allow yourself to have difficult days. Allow yourself to feel frustrated, scared, or sad. These feelings are completely valid. Ask to speak with psychosocial support professionals that may be able to offer additional ideas.
Take Care of Your Mental Health
An extended hospital stay can be emotionally taxing. Loneliness, lack of routine, and frustration with changes in your care plan are some of the most common struggles our care teams help our families face during longer stays.
Ask your care team about additional professional support and resources from art, music, and pet therapy programs to support groups and counseling services. Postpartum Support International (PSI) has a helpline and an app, with resources available in more than 60 languages. The National Maternal Mental Health Hotline is a free resource available 24/7 at 1-800-TLC-MAMA (852-6262) in English and Spanish.